Failed Root Canal Retreatment History
RCT’s (root canal therapies) are a popular conservative treatment for maintaining teeth that would otherwise require extraction. They may save a tooth that has experienced trauma, decay into the nerve or fracture.
Failures can occur, nonetheless, for a variety of reasons, that usually leads to the consideration of having a retreatment.
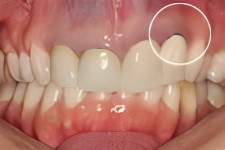
Unfortunately, there are rare cases where an RCT retreatment can show signs of failure and pose risk for compromising adjacent hard and soft tissues (bone, gums, teeth).
In the photo to the right the young lady had two teeth splinted together which led to bone loss between the teeth. Then the lateral incisor fractured and troubles escalated from there.
Representative Case History Example
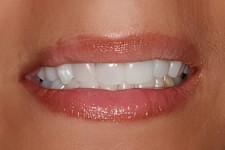
The case presented here is of a young female who had undergone 4 anterior root canals, complete with new porcelain crowns on each tooth.
The adjacent pictures reveal a tinting effect on the gingiva within the immediate vicinity of the root canaled teeth. This is metal showing from the edge of the crown.
One tooth in particular (far right) has compromised bone tissue which was caused, in part, by connecting it to the tooth next to it.
Insufficient Bone For RCT Retreatment or Immediate Implant
Although a standard 3 unit bridge could be used to provide a cosmetic and functional replacement for the failed tooth… the patient instead preferred treatment that would recreate the lost bone to provide a firm foundation for a dental implant replacement.
Chin Block Grafting
The most efficient means for replacing lost bone tissue, for this patient, is a graft of a solid piece of bone.
Although a variety of sources exist for different types of bone (bovine, hip, synthetic, cadaver, etc), more and more bone grafting specialists prefer autogenous bone (patient is the donor) that closely represents the cellular characteristics of the treatment area.
For this area of the jaw, a patient’s chin bone provides an adequate volume of bone for the dental implant’s stability and support. A block of bone is removed from the chin which heals quite rapidly.
The block is measured to specifically “fit” the area needing the graft.
The block of bone provides a biocompatible matrix so blood vessels can form and help to provide a union between the graft and the donor site.
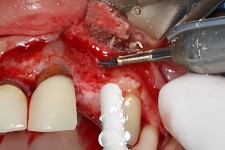
Bone Graft
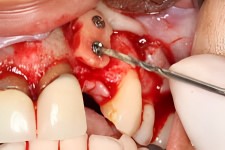
Firm Attachment with Titanium Screws
As can be seen in the adjacent photo, the solid piece of bone is inserted into the treatment area of the future dental implant site.
The width of bone for this implant area will stay within the roots of the adjacent teeth.
Once affixed, additional bone grafting material is inserted into the overall treatment area that will regenerate a flush tissue surface that is natural in appearance.
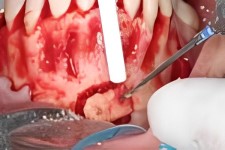
Autogenous Graft Material
Guided Tissue
Regeneration (GTR)
The additional bone graft product is manually placed and packed into all tissue areas to assure that all voids and recesses are filled in to prevent an ingrowth of soft tissue in the graft. If soft tissue gets between the graft and host bone the graft will fail and need to be removed.
A Guided Tissue Regeneration membrane is then used to cover the area that serves to control the overall tissue regeneration process.
The adjacent picture shows how a large segment of sized GTR membrane extends up and under the perio flap (loosened gum tissue on upper arch) that was created to expose the bony ridge. The entire graft area is covered.
Periodontal suturing is performed to reattach the perio flap into it’s original position and also completely covers the extraction and bone graft site.
Tissue regeneration begins immediately. In about 3 months time the treated area regenerates into a solid piece of bone.
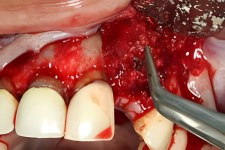
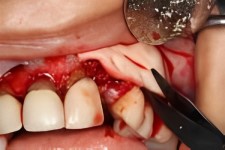
A New Healthy Dental Implant Site
The close up picture provided here shows a healthy reattachment of the perio flap that was created during the bone graft surgery. The titanium screws are no longer needed since the grafted chin bone is now an integral part of the bony ridge.
Implant site development begins with the use of a series of graduated implant drill sizes to sequentially create an implant site that matches the specifications of the implant device.
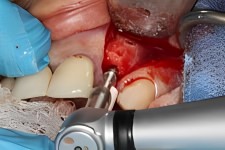
Special attention is exercised to assure that no over-heating of the newly grafted bone occurs. The use of several implant bits provides the extra assurance that this potential error is eliminated.
Depth Adjustment and Temporary Crown
The implant has been successfully seated into the new bone. Osseointegration begins again that will fully integrate the implant device into the jawbone.
The patient elected to have a temporary crown (taken out of occlusion to protect tissues) to eliminate the “toothless” effect.
The small perio flap that was required to expose the titanium screws and the bony ridge as part of the implant surgery is sutured for a second time.
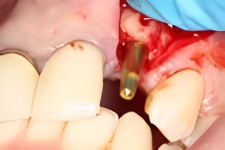
Notice how the overall tissues areas and surface have a nice plump appearance, recreating what Mother Nature originally provides.
Osseointegration Part Two
During this final phase of osseointegration whereby the implant is fully integrated into the newly augmented bone, the remaining three crowns to the right of the newly implanted tooth were carefully removed and replaced with temporaries.
Color matching, for this patient, involved selecting the correct shade that will best match the patient’s adjacent natural teeth and also the abutment that will be used on the new implant.
These extra steps assure that the final cosmetic result is uniform throughout the upper arch.
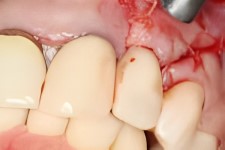
Final Restorative Treatment
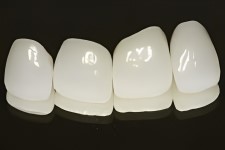
After completing the second phase of implant osseointegration (about 5-6 months) the final restorative crowns are ready for placement.
The technical data necessary for correct color matching and final bite characteristics was developed during this final stage of healing.
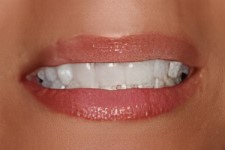
Since all four (4) central anterior teeth were being fully restored, smile line correction performed by Dr. Winter created a cosmetic result that was quite dramatic for the patient.
Treatment Summary
Root Canal Therapy has been an conservative treatment that is quite effective… most of the time.
Events, bite characteristics and tissue conditions nonetheless can and will affect the long term outcome of a successful root canal.
For this particular patient, an eventual treatment failure occurred that affected what most dentists consider to the most important component of dentistry…. bone tissue.
The patient’s deliberate decision to rebuild what was lost… beginning at tissue level, rather than rely on prosthetic alternatives (e.g., bridgework, partials) enabled her to regain nearly everything that was lost with an outcome that would even fool Mother Nature.

Call 414-464-9021 for information on any of our services.
Check out our Dental Blog >>
Read our Patient Case Studies >>
Hampton Dental Associates is proud to offer affordable dentistry programs to help you regain your perfect smile.
Learn more about our affordable dentistry options.