Actual patient that we have kept smiling for 35 years! From crowns and fixed bridge work to implant rehabilitation. Click here to read her story.
Collapsed Bite Reconstruction in Milwaukee, WI
Cosmetic – Functional Facelift
Wear and tear, a normal process, accumulates as we all age. As we approach middle age and beyond, the tell tale signs begin to appear. As our teeth become shorter and shorter, the height of our bites also become shorter and alter the resting positions of our jaws.
Collapsed Bite Rehab Wisconsin For some individuals the wear and tear can become accelerated due to other issues including severe bruxism, periodontal disease, excessive extractions and a variety of untreated traumas.
The cosmetic and functional changes, if left untreated, produce the effect of making us appear older than our natural years. Our smiles collapse, causing our lip structures (especially the upper lip) to flatten out or even sink in.

In time, facial structures begin to appear more rounded or squared off. In severe cases, significant under bite will occur.
The resting position of the jaw also closes… further accentuating an aging mouth structure.
Our featured patient, Fred, had a history of several restoration failures on his upper (maxilla) jaw.
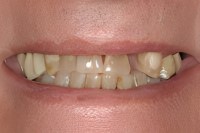
The adjacent pretreatment picture shows the extent of his worn out teeth, along with several distortions of upper tooth structures caused by the ever-changing malocclusion.
Originally, our patient wanted only to repair one tooth…. a tooth that had been repaired several times before.
As Fred became aware of the extensive malocclusions existing between several teeth, he decided to treat the overall problem affecting his entire mouth and jaw structure… rather than a single tooth.
Fred’s new goal was to recreate normal occlusion again… something he hadn’t had for some time.
While Fred focused on having teeth with proper occlusal relationships (fit good – feel good) that would forever end the breakage problem and enable him to eat anything he wanted with self assurance, Dr. Winter created teeth replacement elements that would simultaneously look good and recreate a bite height and normal jaw positioning he hadn’t had in many many years.
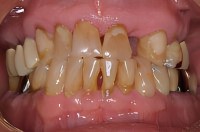
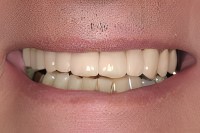
The extreme closeup photo of his upper and lower jaws show the extent of damage and need for a variety of restorative and tooth replacement procedures.
Malocclusion seemingly appears to have affected nearly every upper and lower tooth pair.
The severe wear that had given him an edge to edge bite had worn his incisal edges thin, leading to a bite that was so tight that teeth were now fracturing. He had lost 2 upper left molars before losing his lateral incisor.
Dr. Winter provided the patient with a menu of treatment choices that would address the entire upper jaw and achieve Fred’s goal of getting everything back to normal, the way it is supposed to be and last for a long time.
Once the diagnostic wax-up was completed, Dr. Rick created a set of temporaries that Fred could wear for opening his bite and normalizing his occlusion. These custom temporaries allowed Fred to “test” his new bite and new jaw positions and to also test for correct speech patterns.
The revised temporaries generated the technical data needed by Dr. Rick and his ceramist for fabricating the custom crowns.
The crowns were specially made of Creation porcelain that was layered on gold copings which resulted in a “warmth” of color that was age appropriate for Fred. He did not want the smile of a 20 year old but rather of a 50 year old man.
Fred was very focused on normal dental function… something he hadn’t had in years. He was looking forward to being able to eat and chew all of his favorite foods again…. especially Tagalach – a tasty Jewish baked honey donut!
With a brand new smile and renewed bite we will finish a few crowns on the lower jaw and place implants where he lost 2 upper molars to complete his occlusal rehabilitation.

Call 414-464-9021 for information on any of our services.
Check out our Dental Blog >>
Read our Patient Case Studies >>
Hampton Dental Associates is proud to offer affordable dentistry programs to help you regain your perfect smile.
Learn more about our affordable dentistry options.